Sleep Apnea and Heart Disease: Exploring the Link and Treatment Strategies
Sep 8th 2023

The silent night is shattered by a startling snore, but sleep apnea presents more than just night disturbances - its insidious link with heart disease might be a profound concern. Unraveling this intricate connection requires understanding its profundity, from negligible nocturnal nuisances to seemingly inevitable cardiovascular complications. Join us as we unfold the mysteries of sleep apnea and heart disease, untangle their hidden link, and outline modern treatment strategies that save lives under darkness. The stakes are high; your heart health is on the line even as you slumber. Prepare to dive into a wealth of knowledge and arm yourself against these twin foes in the fight for quality sleep and a healthy heart.
Sleep apnea has been shown to increase the risk of several types of cardiovascular disease, including high blood pressure, stroke, coronary artery disease, and heart failure. This is because it interrupts normal breathing patterns during sleep, which can lead to decreased oxygen levels in the body and strain the heart. It is important to seek medical treatment for sleep apnea if you suspect you have this condition to manage your cardiovascular health and reduce your risk of associated complications.
Understanding Sleep Apnea

Sleep apnea is a sleep disorder characterized by repetitive interruptions in breathing during sleep. These pauses in breathing can range from a few seconds to several minutes and occur multiple times throughout the night. This interruption of airflow happens when the upper airway becomes partially or completely blocked, leading to decreased oxygen levels in the body. As a result, individuals with sleep apnea often experience fragmented sleep, leading to excessive daytime drowsiness and fatigue.
Imagine trying to have a restful night's sleep while constantly waking up due to interrupted breathing. It is no wonder that people with sleep apnea often wake up feeling exhausted instead of refreshed.
There are two main types of sleep apnea: obstructive sleep apnea (OSA) and central sleep apnea (CSA). OSA is the most common form, occurring when the muscles in the throat relax and collapse during sleep, causing a blockage in the airway. Conversely, CSA is less common and occurs when there is a communication problem between the brain and the muscles responsible for breathing.
Untreated sleep apnea can have serious health consequences. Individuals with this condition are at an increased risk for developing various health conditions such as high blood pressure, heart disease, stroke, diabetes, and obesity. Therefore, it is crucial to recognize the signs and symptoms of sleep apnea to seek appropriate diagnosis and treatment.
Now that we understand what sleep apnea is let's explore the causes and symptoms associated with this sleep disorder.
Causes and Symptoms
Sleep apnea can have various underlying causes contributing to its development. One major factor is obesity or excess weight, as fatty tissues in the throat can obstruct airflow during sleep. Other risk factors include anatomical abnormalities such as enlarged tonsils or adenoids, a narrow throat or airway, or a family history of sleep apnea. Lifestyle factors like smoking, alcohol consumption, and sedative use can exacerbate the condition.
Sleep apnea symptoms can vary among individuals. Still, common signs include loud snoring, gasping or choking sensations during sleep, morning headaches, dry mouth or sore throat upon waking, excessive daytime sleepiness, difficulty concentrating or remembering, irritability, and restless sleep. It is important to note that not everyone who snores has sleep apnea, but snoring should be considered a potential indicator of the condition.
Think of sleep apnea as a silent saboteur that slowly chips away at your well-being. Just like a leak in a boat can lead to its eventual sinking if left unattended, untreated sleep apnea can gradually damage your health and quality of life.
If you suspect you or someone you know may have sleep apnea based on these symptoms, it is essential to consult a healthcare professional for an accurate diagnosis. They will assess your medical history, conduct a physical examination, and recommend a sleep study (either in-lab or portable monitoring) to confirm the presence and severity of the condition.
- According to a study from the National Sleep Foundation, individuals with obstructive sleep apnea have a 58% higher chance of developing heart-related complications compared to those without respiratory disorders.
- The same study also noted that nearly 60% of people diagnosed with sleep apnea already had cardiovascular disease.
- The American Heart Association estimates that almost 70% of individuals who have survived a stroke or mini-stroke suffer from obstructive sleep apnea.
Diagnosis and Treatment Options
Healthcare providers typically evaluate patients' symptoms and sleep history when diagnosing sleep apnea. Sometimes, they may refer individuals to a sleep disorder center for further assessment. Diagnostic tests for sleep apnea include nocturnal polysomnography and home sleep tests.
Polysomnography is considered the gold standard for diagnosing central sleep apnea, where the brain fails to send proper signals to the muscles that control breathing. This test involves monitoring various parameters during an overnight stay in a sleep lab. It records brain activity, eye movements, heart rate, blood oxygen levels, and muscle activity to evaluate the severity of sleep apnea.
Home sleep tests are often used as an alternative to polysomnography for obstructive sleep apnea cases. These tests involve wearing portable devices that monitor breathing patterns, heart rate, airflow, and blood oxygen levels while sleeping at home. Home sleep tests are more convenient and cost-effective but may not capture comprehensive data compared to polysomnography.
Once diagnosed with sleep apnea, several treatment options are available depending on the severity of the condition and individual circumstances. Lifestyle changes can be effective for milder cases of obstructive sleep apnea. Weight loss, quitting smoking, avoiding alcohol before bedtime, and sleeping on your side can help alleviate symptoms.
Continuous positive airway pressure (CPAP) machines are commonly prescribed for moderate to severe obstructive sleep apnea. CPAP therapy involves wearing a mask that delivers a steady stream of air pressure to keep the airway open during sleep.
A patient named Mark was diagnosed with severe obstructive sleep apnea after undergoing a polysomnography test. His doctor prescribed a CPAP machine tailored to his needs and assisted in adjusting to its use. Within weeks, Mark experienced improved quality of sleep and reduced daytime fatigue.
In certain cases where CPAP therapy is not well-tolerated, alternative airway pressure devices like auto-CPAP or bilevel positive airway pressure (BPAP) are considered. These devices deliver varying pressure levels during inhalation and exhalation to enhance comfort.
For those who prefer non-invasive options, oral appliances can be used. These devices are custom-made to fit the mouth and help keep the throat open during sleep. While typically recommended for mild to moderate obstructive sleep apnea, oral appliances may also be combined with other treatments for severe cases.
In very rare instances where other treatments have failed or in specific anatomical conditions, surgery may be an option. Surgical procedures for sleep apnea aim to remove or shrink excess tissues, reposition the jaw, or create new openings in the upper airway. However, it's important to note that surgery is often considered a last resort due to potential risks and limitations.
Now that we’ve explored the diagnosis and treatment options available for sleep apnea, let's dive deeper into the link between sleep apnea and heart disease.
- Sleep apnea can be diagnosed through various tests such as polysomnography and home sleep tests, and there are several treatment options available depending on the severity of the condition. Lifestyle changes, CPAP machines, oral appliances, and surgery are all viable options for treating sleep apnea. Addressing this condition is crucial since untreated sleep apnea can lead to more severe health issues like heart disease.
The Link Between Sleep Apnea and Heart Disease

Sleep apnea and heart disease share an intimate connection, with research consistently highlighting their interdependencies. Obstructive sleep apnea, characterized by repeated breathing interruptions during sleep, has been associated with an increased risk of cardiovascular problems.
The frequent pauses in breathing lead to low oxygen levels in the blood and disruption of normal sleep patterns. These factors contribute to the development of high blood pressure (hypertension), irregular heart rhythms (arrhythmias), coronary artery disease, heart failure, and stroke.
One study analyzed data from over 4,500 middle-aged and older adults to identify features of obstructive sleep apnea that could explain its association with cardiovascular disease. It found that reduced blood oxygen levels, known as hypoxic burden, were significantly linked to a higher risk of primary cardiovascular events.
Sarah, a 55-year-old woman diagnosed with moderate obstructive sleep apnea, experienced several episodes of irregular heart rhythms. Through discussions with her healthcare provider and further investigation, it was determined that her sleep apnea contributed to the heart arrhythmias. Addressing her sleep apnea with appropriate treatment reduced the frequency and severity of these issues.
Airway obstruction, a common characteristic of obstructive sleep apnea, accounted for a significant portion of the observed risks. This emphasizes the importance of addressing the underlying causes of sleep apnea to mitigate cardiovascular complications.
Think of the link between sleep apnea and heart disease as a vicious cycle: sleep apnea contributes to heart problems while existing heart conditions can worsen the symptoms and severity of sleep apnea.
By treating sleep apnea effectively, individuals can reduce their cardiovascular risk and improve overall heart health. Prompt intervention enhances quality of life and may prevent potentially life-threatening events associated with heart disease.
The Role of Low Oxygen Levels
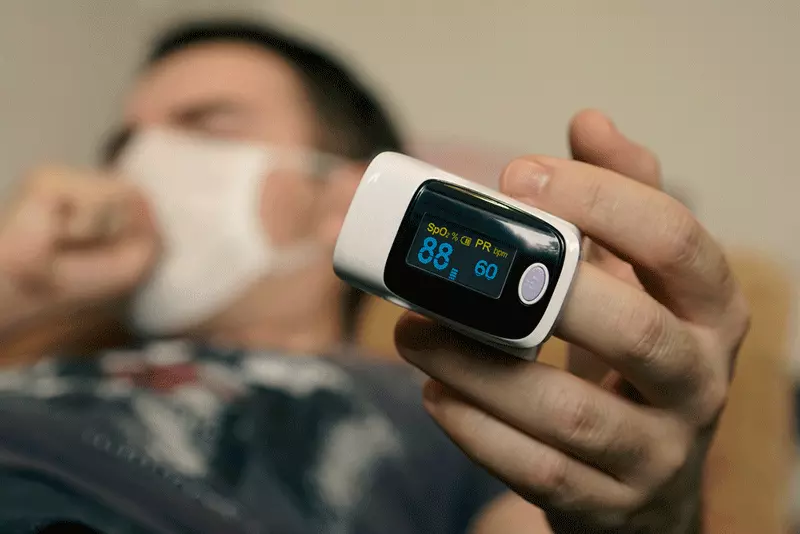
One key factor linking sleep apnea and heart disease is the detrimental effect of low oxygen levels during interrupted breathing. When a person with sleep apnea experiences airway obstruction during sleep, their airflow is limited or completely blocked. As a result, the oxygen levels in their body decrease, leading to a condition called hypoxemia.
In a normal sleep pattern, our body rejuvenates itself by going through different stages of sleep, including rapid eye movement (REM) sleep. However, for individuals with sleep apnea, these crucial stages can be disrupted due to periods of oxygen deprivation. This continuous cycle of low oxygen levels followed by a sudden influx can place excessive stress on the cardiovascular system, triggering various health issues, including heart disease.
To understand this further, let's consider an analogy. Imagine you’re driving your car on a highway. Suddenly, there is construction work ahead, causing traffic to halt. Your car's engine must work harder to keep running and overcome obstacles. Now, envision this happening repeatedly throughout your journey. Eventually, it would take a toll on your car's engine and potentially cause damage. Similarly, the interruptions in breathing and subsequent low oxygen levels strain your cardiovascular system over time.
With each interruption in breathing, your heart must compensate for the lack of oxygen by pumping blood more vigorously and rapidly. If left untreated, this increased workload can lead to conditions like high blood pressure, arrhythmias, and even heart failure.
Consider Mary, a middle-aged woman experiencing symptoms of fatigue, daytime drowsiness, and frequent awakenings at night. After undergoing sleep tests at a clinic, she was diagnosed with moderate obstructive sleep apnea. Mary's doctor explained that her low oxygen levels at night put additional stress on her heart and raised her risk of developing heart disease if the condition remained unaddressed.
Now that we understand the role of low oxygen levels in sleep apnea-related heart disease let's explore how we can identify individuals who are at risk.
Identifying Those at Risk
Sleep apnea is a widespread yet underdiagnosed condition. Many individuals might have sleep apnea without even realizing it. Thus, identifying those at risk is crucial for early detection and intervention.
Several factors can increase a person's likelihood of having sleep apnea:
- Obesity: Excess weight and fat deposits around the neck area can contribute to airway obstruction during sleep.
- Advanced age: Sleep apnea becomes more prevalent as individuals age, with middle-aged and older adults being at higher risk.
- Gender: Men have a higher incidence of sleep apnea than women, although the risk for women increases after menopause.
- Family history: Having close relatives with sleep apnea or other respiratory conditions increases the chances of developing the disorder.
- Certain anatomical features: Structural abnormalities like a deviated septum or large tonsils can obstruct the airway during sleep.
It’s important to note that these risk factors don’t guarantee that someone has sleep apnea but rather indicate an increased likelihood.
Consider John, a 45-year-old man struggling with excessive snoring and daytime fatigue for years. After his father was diagnosed with sleep apnea and heart disease, John became aware of his heightened risk factors due to his family history. Concerned about his health, he decided to consult a sleep specialist who conducted further tests and confirmed his diagnosis.
While some individuals may have obvious signs and symptoms, others may not exhibit any noticeable indicators. This is why it’s crucial to be mindful of common risk factors and personal circumstances when evaluating one susceptibility to sleep apnea-related heart disease. Consulting with a healthcare professional and undergoing proper diagnostic tests can help determine the presence of sleep apnea and accurately assess the risk level.
Now that we’ve discussed identifying those at risk let's explore preventive measures one can take to mitigate the potential impact of sleep apnea on heart health.
Preventive Measures against Sleep Apnea-related Heart Disease

Sleep apnea is a serious sleep disorder that affects sleep quality and poses a heightened risk for heart disease. Recognizing this link, taking preventive measures to reduce the potential impact on cardiovascular health becomes crucial. By effectively addressing and managing sleep apnea, individuals can lower their risk of developing heart-related issues. Let's explore some preventive strategies that can be taken to mitigate the risk of sleep apnea-related heart disease.
The first and perhaps most essential step is to seek professional medical help. Consulting with a healthcare provider specializing in sleep disorders will enable an accurate diagnosis and appropriate treatment plan. They may recommend undergoing a sleep study to confirm the presence of sleep apnea and determine its severity, often through polysomnography or home sleep apnea testing.
Once diagnosed, one of the primary methods to manage and prevent sleep apnea-related heart disease is through continuous positive airway pressure (CPAP) therapy. This treatment involves wearing a mask or nasal device during sleep, which delivers pressurized air to keep your airways open. By maintaining adequate oxygen levels throughout the night, CPAP helps alleviate the interruptions in breathing associated with sleep apnea, reducing cardiovascular strain.
For instance, let's consider John, diagnosed with moderate obstructive sleep apnea. His doctor recommends using a CPAP machine during his nightly sleep routine. With regular adherence to CPAP therapy, John ensures his airways remain unobstructed, preventing fluctuations in blood oxygen levels. As a result, he significantly reduces his risk of cardiovascular complications while enjoying restful nights of uninterrupted sleep.
Besides CPAP therapy, certain lifestyle modifications are crucial in managing and preventing heart disease associated with sleep apnea. One such modification involves maintaining a healthy weight through exercise and balanced nutrition. Obesity is commonly linked to sleep apnea and heart disease, so shedding excess pounds can significantly reduce the severity of sleep apnea and lessen the impact on cardiovascular health.
However, weight management is not the only lifestyle factor to consider. Addressing other risk factors such as smoking, excessive alcohol consumption, and sedentary behavior are equally important in reducing the risk of sleep apnea-related heart disease.
Smoking damages the blood vessels and increases inflammation, exacerbating cardiovascular risks already heightened by sleep apnea. Quitting smoking can significantly improve overall heart health and decrease the severity of sleep apnea symptoms.
Moreover, limiting alcohol intake is crucial as alcohol relaxes the muscles in the throat, making it more likely for breathing difficulties to occur during sleep. By practicing moderation or abstaining from alcohol consumption, individuals can improve their sleep quality and reduce their risk of heart disease.
Regular physical activity is another key preventive measure against sleep apnea and heart disease. Exercise helps maintain a healthy weight, strengthens the cardiovascular system, and enhances respiratory function - all essential components for reducing the impact of sleep apnea on heart health. Incorporating activities that elevate heart rate and challenge the lungs regularly contributes to an overall healthier lifestyle.
By seeking medical attention promptly, adopting CPAP therapy when necessary, embracing a healthy lifestyle with proper weight management, quitting smoking, moderating alcohol consumption, and engaging in regular exercise, individuals can take proactive measures to prevent sleep apnea-related heart disease. Remember, every step taken towards ensuring adequate sleep and promoting cardiovascular wellness lays a foundation for a healthier life overall.
